What is PBM?
To download this video, with or without subtitles, please right-click on one of the following links and select "Save Link As..." (Chrome and Firefox), "Save target as..." (Internet Explorer), "Save linked content as..." (Opera) or "Download Linked File As..." (Safari).
- Low Quality (MP4, 480p):
 With Subtitles (5.82 MB)
With Subtitles (5.82 MB) - Medium Quality (MP4, 720p):
 With Subtitles (6.82 MB)
With Subtitles (6.82 MB) - High Quality (MP4, 1080p):
 With Subtitles (7.82 MB)
With Subtitles (7.82 MB)
What is the Evidence telling us?
To download this video, with or without subtitles, please right-click on one of the following links and select "Save Link As..." (Chrome and Firefox), "Save target as..." (Internet Explorer), "Save linked content as..." (Opera) or "Download Linked File As..." (Safari).
- Low Quality (MP4, 480p): With Subtitles (37MB), Without Subtitles (35MB)
- Medium Quality (MP4, 720p): With Subtitles (68MB), Without Subtitles (64MB)
- High Quality (MP4, 1080p): With Subtitles (139MB), Without Subtitles (142MB)
Quick links to sections on this page:
Patient Blood Management Guidelines
What are the PBM Guidelines?
To download this video, with or without subtitles, please right-click on one of the following links and select "Save Link As..." (Chrome and Firefox), "Save target as..." (Internet Explorer), "Save linked content as..." (Opera) or "Download Linked File As..." (Safari).
- Low Quality (MP4, 480p): With Subtitles
- Medium Quality (MP4, 720p):
 With Subtitles (7.05 MB)
With Subtitles (7.05 MB) - High Quality (MP4, 1080p):
 With Subtitles (8.38 MB)
With Subtitles (8.38 MB)
Visit Patient Blood Management Guidelines to access the latest modules in the Guidelines or click on the images below to go directly to the relevant module.
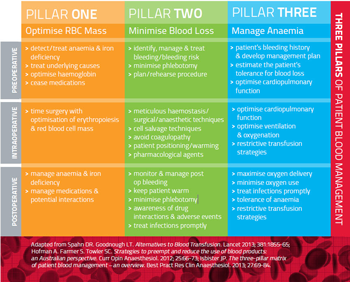
Patient Blood Management improves patient outcomes by improving the patient’s medical and surgical management in ways that boost and conserve the patient’s own blood. As a consequence of better management, patients usually require fewer transfusions of donated blood components thus avoiding transfusion-associated complications. The National Blood Authority is funding and managing the development of evidence-based, Patient Blood Management Guidelines. A multidisciplinary team determines, with the patient, the specific management plan, which makes every reasonable endeavour to optimise the patient’s own blood volume, minimise blood loss, and optimise the patient’s physiological tolerance of anaemia. There are various techniques to ensure this. For example, the Three Pillars of PBM [1] model depicted below helps to show how various practices can be initiated during pre-, intra- and post-operative stages of surgery.
The rationale for patient blood management addresses evidence-based transfusion medicine practice and stewardship of donated blood, to:
- view a patient’s own blood as a valuable and unique natural resource that should be conserved and managed appropriately
- acknowledge that altruistically donated blood is a valuable, unique and costly resource that is held in trust, and that it will only be used as therapy when there is evidence for potential benefit and potential harm will be minimised
- consider transfusion alternatives
- ensure quality products are available in a timely and safe manner
- ensure potential hazards are considered and balanced against the benefits, and
- explain the benefits and risks to the patient/relatives.
Implementing the PBM Guidelines
Visit Implementing the Patient Blood Management Guidelines to access the latest tools and information to support health providers implementing PBM strategies. On this page you will also find the NBA's National Patient Blood Management Implementation Strategy 2017-2024.
Patient Blood Management Advisory Committee (PBMAC)
The Patient Blood Management Advisory Committee replaces the previous Patient Blood Management Steering Committee. The Patient Blood Management Advisory Committee (PBMAC) was established in 2019 to provide advice and guidance to the NBA in relation to the implementation of PBM in Australia consistent with the NBA's responsibilities specified in the National Blood Authority Act 2003 and the ![]() National Blood Agreement (135.16 KB).
National Blood Agreement (135.16 KB).
The committee was established by the NBA Chief Executive under Section 38 of the National Blood Authority Act 2003 and is comprised of individuals with expertise and knowledge in the health sector, blood management, education, quality and safety, and consumer issues.
The PBMAC Terms of Reference (ToR), the PBMAC Membership and Section 38 Instrument are approved by the NBA's Chief Executive and detail the governance arrangements.
- PBMAC terms of reference (pdf)
- PBMAC terms of reference (docx)
- PBMAC Membership (pdf)
- PBMAC Membership (docx)
- Instrument of establishment under s38 PBMAC (pdf)
- Instrument of establishment under s38 PBMAC (docx)
For more information